Integrating the life-stages approach to increase demand for immunisation through a human-centred design (HCD) methodology: lessons learned from Somalia
Highlight box
Key findings
• Engaging communities in assessment and planning of health services using human centred design (HCD) approach allowed communities to have a say on immunisation services and address barriers to immunisation.
• Engaging female health workers addressed gender barriers to immunisation and allowed mothers to bring their children for immunisation.
• Integration of health service provision using life stages approach allowed communities in hard-to-reach areas to access immunisation and other health services in a “one-stop shop”.
What is known and what is new?
• Delivery of health services in a setting with ongoing conflict, like Somalia, is challenging. Lack of access to health services, including immunisation may lead to future disease outbreaks. Facilitating participation of communities in assessment and planning of health services is a challenging task. In a heavily patriarchal society, female caregivers (mothers) may be reluctant to access health services from male healthcare providers (such as vaccinators)
• Communities participated in assessment of issues and planning of health services, which reduced barriers to access to the same, including immunisation. The work also strengthened participation of women in delivery of immunisation services, which addressed gender barriers to access to services owing to the heavy patriarchal customs in Somalia.
What is the implication, and what should change now?
• Planning and delivery of health services in conflict settings requires participation of communities using an HCD, and integration of services through a life-stages approach to facilitate inclusion of vulnerable groups and access to all services in a “one-stop shop” setting.
Introduction
Somalia lies in the north-east of Africa, otherwise called the Horn of Africa, and is bordered by Kenya, Ethiopia, Djibouti, the Gulf of Aden/Red Sea, and the Indian Ocean. It is home to over 17 million people (2022 estimate), who mostly rely on livestock farming and diaspora remittances to earn their living (1).
Somalia has a total fertility rate of 6.9 children per woman (2020 situation, which seems to remain the same over the years). Women get married at a young age, with 36 percent of women aged 20–24 years having married before the age of 18 years, and 27% of women start bearing children by the age of 18 years (1). Somalia has a high maternal mortality ratio of 692 deaths per 100,000 live births. This is, in part, because only about 24 percent of pregnant women aged 15–49 years complete the recommended minimum of four antenatal care (ANC) visits during pregnancy, and only 32 percent of women deliver their babies with a skilled birth attendant.
A further lower percentage of women deliver at health facilities (currently at 21 percent), and only 11 percent of women had a postnatal check within two days of delivering a baby, with only 10 percent of babies also undergoing the check within two days (1). Even after childbirth, only 11 percent of children aged 11–23 months receive all requisite vaccinations, with up to 60 percent of children having not received any vaccinations at all (zero dose) (1). According to United Nations Children’s Fund (UNICEF), Somalia’s under-five mortality ratio stands at 115 per 1,000 live births. Further, 37 newborns die for every 1,000 born, and 73 infants out of every 1,000 die (2).
The Somali Government’s maternal health vision is to reduce maternal mortality and morbidity by ensuring that all Somali people have access to quality healthcare without suffering financial burden. However, many years of political unrest and conflict in Somalia have led to challenges in multiple social sectors, including the health system, which is reflected in the health indicators for the country. This is attributable partly to a lack of adequate resources for healthcare delivery and inadequate data to support planning. Reproductive health indicators are the worst hit. The prevailing emergency context in Somalia makes it difficult for inclusion and participation of communities in identifying and addressing key drivers of their poor health. Communities are often a passive recipient of decisions made on their behalf by the government, and planning and delivery of health services is a one-way, top-down process (3).
To address some of the key drivers of poor reproductive, maternal and child health, a human centred design (HCD) approach was used during the development of the social and behaviour change (SBC) strategy for reproductive, maternal, newborn, child, and adolescent health (RMNCAH) in 2023–2027. The objective of employing HCD was to facilitate inclusion and participation of communities in assessment, planning and implementation processes to understand and address key drivers of RMNCAH in Somalia. This paper documents how the strategies were employed in immunisation interventions, a key component of RMNCAH.
Methods
This project, which spanned from 2022 to 2024, utilised four interrelated models and frameworks: the Journey to Health and Immunisation (JTHI) framework, HCD and the Socio-Ecological Model (SEM) for analysis and the life stages approach (LSA) for implementation. To understand factors affecting immunisation in Somalia, we utilised the JTHI framework, developed by UNICEF (Figure S1) to promote a holistic understanding of the immunisation process as various stages of immunisation (4).
To gain a better understanding on behavioural drivers of immunisation especially among women, a gender and immunisation barriers assessment was conducted in high-risk priority districts (district that are hard to reach due to ongoing armed conflict) among vulnerable populations (including hard to reach populations such as people with disabilities, nomadic farmers, internally displaced populations and people cut off from normal service delivery due to ongoing armed conflict). The analysis indicated disparities in vaccine uptake and access to health services among vulnerable populations, with women, girls, and persons with disabilities being disproportionately affected (5). This analysis complements the HCD findings, indicating that gender expectations and norms lead to disparities in how women, men, girls, and boys are informed about, seek, and access healthcare services and resources (6), and how gender inequalities permeate every stage of the healthcare and immunisation process.
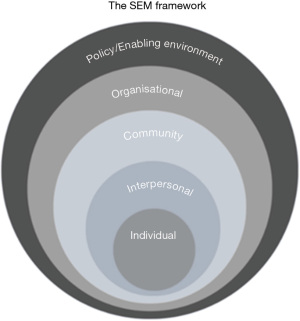
The SEM of SBC (see Figure 1) (7) asserts that human behaviour is not shaped by one factor or one level but by dynamic interrelations of factors in the individual, and among various personal and environmental factors. The SEM asserts that human behaviour is shaped by an interplay of factors from individual (intrapersonal), interpersonal, organisational, community, societal (policies and laws) and the physical “ecological” environment.
The SEM enables a multi-level and multi-stage approach. Each level overlaps with the other, and therefore, considers the continuum of interactions and interplay between and among each level. It uses a cross sectional and holistic approach, which is relevant for a complex issue like RMNCAH. As a multi-level model, the SEM also demands engagement of multiple approaches to behaviour change, such as interpersonal communication, community mobilisation and advocacy. It also engages all relevant stakeholders and participant groups in the commitment to attain sustainable change and development.
To adequately address issues across all levels of the SEM, Somalia employed the use of a life-stages approach to ensure integration of all issues related to RMNCAH (including immunisation), and to achieve a holistic approach to addressing these issues.
LSA
The LSA addresses health issues over a life course and considers the physiological and social milestones that people go through in life. Health issues that people face in life are dependent on the life stage that they are in, and critical periods of time where biological, psychological, and environmental changes occur. LSA addresses health needs for each population segment through their stage of life (Figure S2). Five key life stages are prioritised as critical to addressing health issues related to RMNCAH (including immunisation):
The following key participant groups (otherwise called audiences) were identified for RMNCAH in Somalia:
- Reproductive-age men and women/young couples: men and women, including young people aged 15–24 years old, who may be recently married couples intending to have children.
- Pregnant women (regardless of age)/their husbands: this life stage covers conception to delivery of a child, after which the group members become parents of under-five children (see below).
- Parents/caretakers of under-five children: parents of children who are below 5 years old. Includes men and women from the time that they deliver a baby (from pregnancy), to the time that the child is 5 years old. Alternatively, caretakers of children (who are doing so on behalf of parents) are also included in this category. Subgroups in this category include parents/caretakers of newborns (children aged 0–6 months); parents/caretakers of children aged 6–23 months; and parents/caretakers of children aged 24–59 months.
- Parents of older children: parents/caretakers of children aged 6–19 years. Subgroups in this category include parents/caretakers of school-going children aged 6–9 years, and parents of adolescents (10–19 years).
- Adolescents: early adolescents (aged 10–14 years) and late adolescents (aged 15–19 years). This group includes adolescents who are in school and those who are out of school. This group also has an overlap with reproductive-age men and women, as, due to social situations, some adolescents in this category may already be married and engaged in childbearing
Ethical considerations
The study was conducted in accordance with the Declaration of Helsinki and its subsequent amendments. For the ethical clearance, the Gender Immunzation Barrier Analysis study (IGBA) was part of the broader UNICEF Gender Programmatic review for Somalia. This did not require external ethical review, but instead the study was subjected to the consultant firm’s internal process (Includovate).
Results
Behaviour and culture issues
Somalia is a heavily patriarchal society, where health-related decisions are influenced by men. Women must seek permission from their husbands (who are often influenced by elder family members, such as mothers-in-law) to seek healthcare, including attending antenatal services, delivery of babies at health facilities (including caesarean section) and taking children for immunisation. Women are also financially dependent on their husbands for transportation to access healthcare. Women feel uncomfortable accessing healthcare from male health workers. These factors result in low utilisation of health services by women, including for immunisation.
A recent Immunisation Gender Barrier Analysis (IGBA) reinforced these observations and highlighted this discrepancy: although mothers are the primary caregivers and often initiate healthcare for their children, most women surveyed could not make independent decisions about immunisation. Most required spousal or elder approval. Many mothers expressed willingness to vaccinate their children, but misconceptions and fears often undermined their intent. For instance, some caregivers believed that certain vaccines could cause infertility or other harm, which made them hesitant, particularly in relation to vaccinating daughters. Persons with disabilities and their families were also disproportionately affected: they faced additional barriers such as difficulty travelling to distant clinics, lack of accessible facilities, and limited tailored communication, resulting in lower vaccination uptake in households with members with disabilities compared to others (see Appendix 1 for additional details on findings from gender analysis).
Healthcare delivery challenges
The health system is heavily resource-constrained. Health facilities are far from one another; there is security threat in some areas, making it impossible for government to deliver static healthcare. Some health services are simply not available in some areas, making it impossible for the population to access them. It is not possible for Somalis to access good health care that provides all integrated services in one place, as close as possible to the community, and with minimal out-of-pocket expenditure.
Even though the recruitment of female healthcare workers is intended to address gender barriers in accessing healthcare, they too are impacted by prevailing gender norms, and some women might not prefer the treatment they get from female health workers (8).
Improving access to vaccinations and ensuring that everyone is vaccinated requires understanding how gender norms, roles, and relationships impact vaccination for women, men, girls, and boys, as well as the diversity within these groups. Completing or receiving vaccinations, comprehending the significance of vaccination, having the ability to make vaccine-related decisions, and utilising health services all impact national health outcomes and the health of women, families, and future generations.
Applying HCD to plan for implementation
UNICEF Immunisation Programmes rely heavily on disaggregated data for planning and implementation of demand generation activities for health promotion. Besides the use of data, UNICEF also aligns implementations that are theory-driven to determine underlying paths of social structures, such as the SEM. For sustainability, empowerment, and ownership, using an HCD approach allows communities to be in the driver’s seat. The use of a life stage approach ensures that immunisation programmes leave no one behind, and that the utilisation of existing interfaces between communities and service providers for continuous uptake of health services. Using this mixed approach highlighted the following results:
The data from the National Immunisation Day (NID) in September 2024 underscored several gender-related challenges:
- Vaccination team composition: gender composition in vaccination teams varied from region to region. While vaccination teams were predominantly female, a deliberate strategy designed to facilitate better interaction with mothers and caregivers, in regions such as Baidoa and Kismayo, culturally driven norms restricting women’s public participation limited female team members’ involvement. These norms include societal expectations for women to primarily remain in domestic spaces, reducing their availability for public health activities. Consequently, male-dominated teams in these areas encountered challenges engaging directly with women, who typically care for children but often do not independently make household health decisions.
- Vaccination coverage: overall coverage among children under-five was 91%, with some regions, like Southwest, reaching 98%. For context, the 2020 Somali Health and Demographic Survey reported that only about 13% of children aged 12–23 months had received all basic vaccines. Thus, reaching 91% of children (even in a one-off campaign) suggests significant progress. While NIDs typically achieve higher coverage through door-to-door outreach, this result also reflects increased community acceptance and participation. It is reasonable to attribute part of this success to the project’s HCD-driven demand generation efforts that addressed prior barriers to vaccination uptake (attribution is inferred because the interventions, such as engaging influencers and female mobilisers, were rolled out before NID-1, directly targeting the causes of low coverage).
- Barriers to access: social mobilisers were the main source of information about the campaign for 90% of households. Female mobilisers were particularly effective in engaging mothers and caregivers, but their absence in conservative regions may have limited outreach efforts.
- Cultural sensitivity and challenges: security concerns and cultural restrictions made it difficult to deploy female vaccination workers in some areas, reducing engagement with women. Parental refusals, influenced by cultural misconceptions about vaccines, further hindered progress, highlighting the need for gender-sensitive health communication strategies.
Review of data from Big Catch-Up (BCU) vaccination exercises (to strengthen routine immunisation reaching high-risk priority areas and vulnerable populations) identified the following gender disparities in vaccination coverage:
- Bacillus Calmette-Guerin (BCG vaccine): facility-based services showed slightly higher coverage for boys, especially in regions such as Afgooye. Outreach services, however, achieved more equitable gender coverage.
- Oral Polio vaccine (OPV): boys had consistently higher coverage in facility settings, with outreach services, again balancing coverage more equitably between boys and girls.
- Pentavalent vaccine [diphtheria, tetanus, pertussis, hepatitis B, haemophilus influenzae type b (DPT-HepB-Hib)]: similar patterns emerged, where boys had higher facility-based coverage, but targeted outreach reduced this gender disparity significantly.
These three vaccines (BCG, OPV, and DPT-HepB-Hib) were selected for detailed gender analysis because they represent critical early childhood vaccines, have comprehensive gender-disaggregated data available, and are indicative of broader vaccination equity challenges. Other vaccines were not analysed in detail due to insufficient gender-disaggregated data in existing campaign reports.
The project’s integrated approach aimed to improve RMNCAH outcomes alongside vaccination, showing promising results: supported districts reported increases in pregnant women attending ANC and facility-based deliveries, critical improvements given Somalia’s very low national averages (only 24% complete 4 ANC visits, 32% skilled births). While it is too early to see significant reductions in Somalia’s alarmingly high maternal (692/100,000) and under-five mortality (115/1,000) rates, the observed upticks in service utilization (preventing childhood illnesses and encouraging safe motherhood/newborn care), address key root causes and signal that the interventions are moving in the right direction, sustained efforts are crucial for future mortality reductions.
Based on the data analysed, the following interventions were reinforced:
- Increased mobile vaccination units in nomadic and rural areas to strengthen routine immunisation;
- Increased engagement with female health workers and community influencers to address cultural barriers;
- Enhanced skills of health workers, especially at points of service, including interpersonal communication;
- Targeted mobilisation and advocacy campaigns aimed at reducing vaccine hesitancy, particularly among women, by involving religious leaders and male advocates for female participation in the decision-making process.
Discussion
The HCD approach is used to put communities actively at the centre of programme planning, prioritisation and implementation. Communities are part of the decision-making process, empowerment, and accountability on issues related to their health, as opposed to being passive recipients of decisions made on their behalf. This approach is key to analysing, understanding and addressing key behavioural issues that affect immunisation programming and interventions to increase uptake of vaccines in female clients and other vulnerable populations.
Applying the SEM helped in identifying key audiences responsible for increasing uptake of immunisation services, as well as their influencers and socio-economic factors that hindered uptake of services. Using SEM helped in determining how the engagement of male vaccinators presented a barrier for access to immunisation services by communities within the Somali patriarchal society.
Using the life-stages approach, where health services were tailored for key stakeholders based on their life stage, facilitated integration of key health services, including immunisation. The healthcare delivery system provided “a one-stop-shop/supermarket” where audiences could access services in one place. Given existing poor health seeking behaviours made worse by access marriers (safety, long distances, availability of health facilities), the chance of getting all services during an outreach session made it easier for communities to access all essential services at once.
Recommendations
- Employing LSA allows integration of interventions to be delivered to communities in a one-stop shop for health services based on audiences, such as new mothers, mothers of under-five children, etc.
- Integration allows a one-stop shop with all services, especially when we get access to certain populations. i.e., access to high-risk priority areas, nomadic due to movement-environmental shocks.
- Utilising HCD allows for inclusion, involvement and active participation of communities and other stakeholders in analysis, prioritisation, planning and implementation of health services, a partnership that brings efficiency and sustainability of interventions.
- Engagement of female health workers in immunisation encourages utilisation of health services, especially in a heavily patriarchal society like Somalia, where mothers are primary caregivers.
Conclusions
Integrating the LSA using HCD in the immunisation work in Somalia showed that, when communities are involved and participate in identifying and addressing issues related to their health, including addressing barriers, it can lead to increased uptake of immunisation services among vulnerable communities, including people living in high-risk areas.
Discussion questions
Given the information and the scenario shared in the case study, in groups, consider the following questions. What would your approach be in designing and implementing interventions using data, social theories, and engagement of communities?
- To address gender-related barriers, identify specific barriers affecting women’s decision-making, participation in immunisation services, and the effect it can have based on community leaders/groups, caregivers, youth, adolescents, and local influencers (refer to Table 1).
- What mechanisms can be put in place to build trust in systems and vaccinations through the SEM? Consider the following linkages that affect immunisation programmes: JTHI, use of the SEM or additional theories or concepts, and data for action.
- Based on the mechanisms you have discussed (in question 2), identify the partners and resources needed to implement your action plan.
Table 1
| Level of implementation | Planning elements | ||||||
|---|---|---|---|---|---|---|---|
| Barriers identified | Focus population | Proposed actions | Target audience | Responsible person | Partners needed | Resources | |
| Individual | |||||||
| Community | |||||||
| Health system | |||||||
| Policy | |||||||
UNICEF, United Nations Children’s Fund.
Acknowledgments
This work received manuscript review and support from Brenda Kambaila, Khadija Abdalla, Fadumo Nour UNICEF Somalia, AAIA, Mogadiscio, Somalia.
Footnote
Provenance and Peer Review: This article was commissioned by the Guest Editor (Mellissa Withers) for the series “Case Studies in Global Health Leadership and Management” published in Journal of Public Health and Emergency. The article has undergone external peer review.
Data Sharing Statement: Available at https://jphe.amegroups.com/article/view/10.21037/jphe-24-109/dss
Peer Review File: Available at https://jphe.amegroups.com/article/view/10.21037/jphe-24-109/prf
Funding: None.
Conflicts of Interest: All authors have completed the ICMJE uniform disclosure form (available at https://jphe.amegroups.com/article/view/10.21037/jphe-24-109/coif). The series “Case Studies in Global Health Leadership and Management” was commissioned by the editorial office without any funding or sponsorship. The authors have no other conflicts of interest to declare.
Ethical Statement: The authors are accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved. The study was conducted in accordance with the Declaration of Helsinki and its subsequent amendments. For the ethical clearance, the Gender Immunzation Barrier Analysis study (IGBA) was part of the broader UNICEF Gender Programmatic review for Somalia. This did not require external ethical review but instead the study was subjected to the consultant firm’s internal process (Includovate).
Copyright Information: This is a work of the United Nations, prepared by staff of UNICEF Somalia in their official capacity. It is therefore in the public domain and may be freely reproduced, quoted, or translated, in part or in full, without permission. However, any dissemination should acknowledge UNICEF as the source.
Open Access Statement: This is an Open Access article distributed in accordance with the Creative Commons Attribution Licence (CC BY), which permits the replication and distribution of the article as long as the original work is properly cited (including links to both the formal publication through the relevant DOI and the license). See: https://creativecommons.org/licenses/by/4.0/.
References
Directorate of National Statistics, Federal Government of Somalia, The Somali Health and Demographic Survey (DHS) 2020 . Available online: https://nbs.gov.so/wp-content/uploads/2023/07/Somali-Health-Demographic-Survey-2020.pdfUNICEF, Somali Multiple Indicator Cluster Survey (MICS) 2011 . Available online: https://mics.unicef.org/surveys- Somali Federal Ministry of Health, Reproductive, Maternal, Newborn, Child and Adolescent Health in Somalia: A strategy for social and behaviour change, 2023-2027. Available online: Improving healthcare services in somalia project ‘damal caafimaad’ stakeholder engagement plan (SEP), 2021. Available online: https://documents1.worldbank.org/curated/en/817611620856125118/pdf/Stakeholder-Engagement-Plan-SEP-Improving-Healthcare-Services-in-Somalia-Project-Damal-Caafimaad-P172031.pdf
- United Nations Children’s Fund. Demand for Health Services: A Human Centered Field Guide for Investigating and Responding to Challenges. 2018. Available online: https://www.unicef.org/innovation/sites/unicef.org.innovation/files/2018-11/demand_for_healthservices_fieldguide.pdf
- International Organisation of Migration: Humanitarian needs overview: Somalia. 2022. Available online: https://somalia.iom.int/sites/g/files/tmzbdl1041/files/documents/IOM%20Somalia%20Infosheet%20Feb%202022.pdf
- Muralidharan A, Fehringer J, Pappa S, et al. Transforming gender norms, roles, and power dynamics for better health: evidence from a systematic review of gender-integrated health programmes in low- and middle-income countries. Futures Group. 2015. Available online: https://www.measureevaluation.org/resources/publications/tr-15-118/at_download/document
- Klasa K, Galaitsi S, Wister A, et al. System models for resilience in gerontology: application to the COVID-19 pandemic. BMC Geriatr 2021;21:51. [Crossref] [PubMed]
- UNICEF. From coverage to empowerment: Integrating gender in immunisation demand. Promising practices from six countries. 2022. Available online: https://www.gavi.org/sites/default/files/2022-10/Integrating-Gender-in-Immunization-Demand-case-studies.pdf
Cite this article as: Shamalla-Hannah L, Kommwa I, Darboe B, Owusu-Aboagye M, Muigai J, Eltayeb AO, Kader M. Integrating the life-stages approach to increase demand for immunisation through a human-centred design (HCD) methodology: lessons learned from Somalia. J Public Health Emerg 2026;10:7.